Podcast: Play in new window | Download (Duration: 15:50 — 14.5MB) | Embed
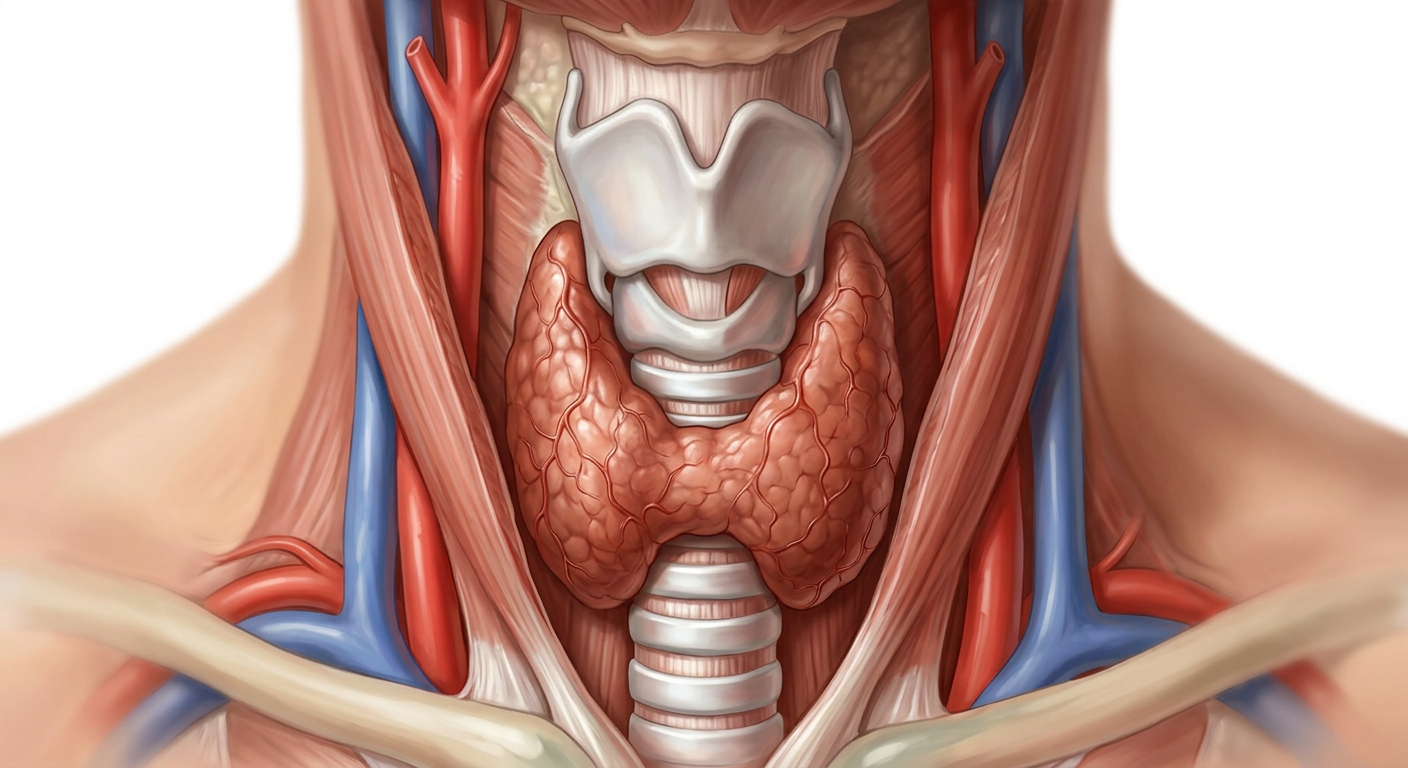
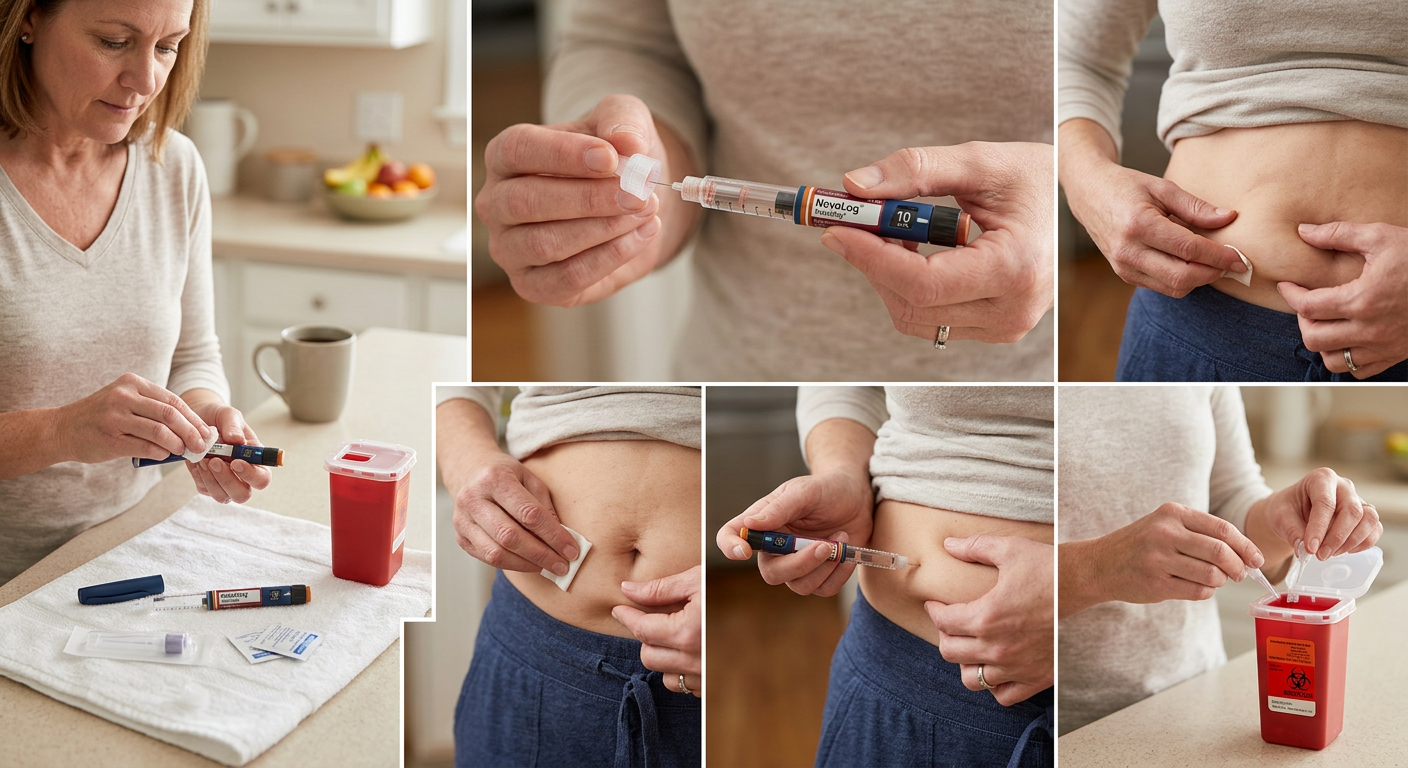
This podcast episode gives nurses a practical, easy-to-apply overview of common thyroid disorders, focusing on how to recognize and manage both hypothyroidism and hyperthyroidism in clinical practice. It reviews key differences in presentation—such as fatigue, weight gain, and cold intolerance in hypothyroidism versus weight loss, tachycardia, and heat intolerance in hyperthyroidism—while connecting these symptoms to underlying physiology. Nurses will learn important medication considerations, including proper administration of levothyroxine and monitoring for adverse effects with methimazole. The episode also highlights critical safety topics like recognizing thyroid storm, interpreting lab values (TSH, T3, T4), and providing effective patient education. With real-world clinical pearls, this episode helps nurses build confidence in managing thyroid conditions across care settings.
Be sure to check out our free Top 200 study guide – a 31 page PDF that is yours for FREE!